How I Diagnosis Long COVID
A Mechanism-Based, Personalized Process
Long COVID is not a single disease with a single cause.
It is a multi-mechanism syndrome, meaning different biological systems can be disrupted at the same time—or in different combinations—in different people.
This is why one medication, one supplement, or one protocol does not work for everyone.
Diagnosis is not about labeling symptoms. It is about identifying which underlying mechanisms are driving those symptoms in your body.
Why Traditional Diagnosis Often Fails in Long COVID
Most conventional approaches search for one explanation:
- Persistent virus
- Autoimmunity
- Anxiety or stress
- Deconditioning
In reality, Long COVID behaves more like a systems failure, not a single pathology.
Two people can share the same symptom—fatigue, brain fog, palpitations—and have completely different causes underneath.
Why Symptoms Alone Are Not a Diagnosis
Imagine you bring your car to a mechanic and say:
“My car won’t start.”
That statement is accurate—but it doesn’t explain why the car won’t start.
A car can fail to start for many different reasons:
- A dead battery
- A failed starter
- A broken fuel pump
- No fuel in the tank
- An alternator problem
- A faulty sensor
The symptom is the same, but the cause is different in every scenario.
If the mechanic replaces the battery without investigating further, the car may still not start—not because the mechanic didn’t try, but because the wrong problem was treated.
Long COVID works the same way.
Symptoms like fatigue, dizziness, pain, insomnia, brain fog, or palpitations are real—but they are descriptions, not diagnoses.
The same symptom can come from different mechanisms:
- Fatigue can be driven by nervous system dysfunction, mitochondrial impairment, hormone imbalance, inflammation, or poor circulation
- Brain fog may arise from dysautonomia, histamine excess, endothelial dysfunction, gut-immune signaling, or disrupted sleep
- Palpitations can be caused by autonomic instability, mast cell activation, hormonal shifts, or vascular dysfunction
Treating symptoms without identifying the mechanism is the equivalent of changing random car parts and hoping something works.
Step 1: Understanding Long COVID as a Multi-Mechanism Syndrome
Step 1: Understanding Long COVID as a Multi-Mechanism Syndrome
Every patient is evaluated through the framework of six core biological mechanisms known to drive Long COVID:
- Dysautonomia / Nervous System Dysfunction
- Mitochondrial Dysfunction
- Endothelial Dysfunction and Microcirculation Impairment
- Histamine Excess / Mast Cell Activation
- Gut Dysbiosis and Immune-Gut Signaling
- Hormone Imbalance
Most patients have more than one mechanism involved. The goal is not to treat everything at once, but to identify which mechanisms matter most.
Symptoms Mapped to their Mechanisms
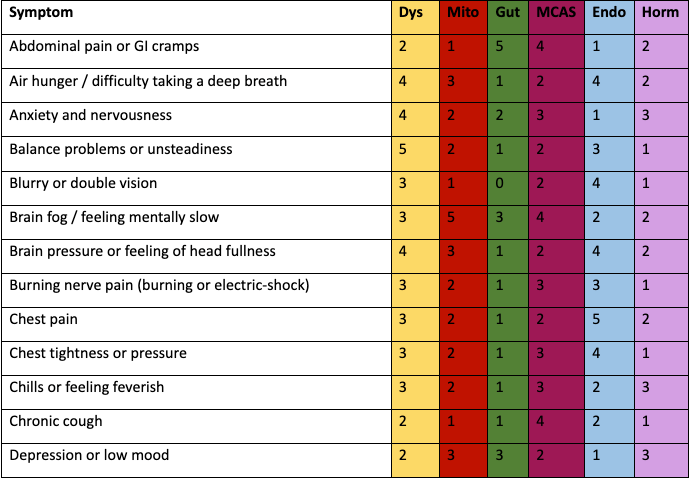
(Dys = Dysautonomia · Mito = Mitochondrial Dysfunction · Gut = Gut Dysbiosis/Leaky Gut · MCAS = Histamine/Mast Cells · Endo = Endothelial/Microclots · Horm = Hormone Imbalance)
Step 2: Using Triggers and Symptoms to Identify Mechanisms
Instead of relying solely on lab tests, I start with something far more informative: how your symptoms respond to specific triggers.
Triggers reveal which systems fail under stress.
Common triggers include:
- Heat or temperature changes
- Physical or cognitive exertion
- Emotional stress
- Poor or disrupted sleep
- Certain foods
- Standing, bending, or posture changes
- Hormonal cycles
Patterns across these triggers allow me to determine which of the six mechanisms are active, and how strongly each contributes.
This step replaces guesswork with prioritization.
Step 3: Targeted Laboratory Testing (When It Adds Value)
Laboratory testing is used to confirm clinical findings, not to search blindly.
Once the involved mechanisms are identified, labs may be ordered to:
- Confirm mitochondrial dysfunction
- Evaluate inflammation or endothelial markers
- Assess hormone imbalances
- Identify gut-immune contributors
- Exclude overlapping or confounding conditions
This approach avoids unnecessary testing while maintaining medical rigor.
Step 4: Designing a Personalized Treatment Plan
Treatment is based on your unique mechanism profile, not a generic Long COVID protocol.
Your plan may include:
- Targeted medications
- Focused supplement strategies
- Nervous system regulation techniques
- Hormonal support
- Gut-immune interventions
- Pacing and lifestyle guidance
The goal is mechanism correction, not temporary symptom suppression.
Step 5: Monthly Follow-Ups and Ongoing Adjustments
Long COVID is not static. As one mechanism improves, another may become more apparent.
Monthly follow-ups allow us to:
- Reassess symptoms and trigger responses
- Identify shifts in dominant mechanisms
- Adjust dosing, timing, or treatment focus
- Remove therapies that are no longer needed
- Introduce new strategies when appropriate
This keeps care precise and avoids overtreatment.
When In-Office Procedures Are Considered
Some patients benefit from procedural interventions, particularly when nervous system dysfunction is a dominant driver.
If dysautonomia is identified as the primary mechanism, treatment may include:
- Stellate Ganglion Block (SGB)
- Epipharyngeal Abrasive Therapy (EAT)
These are selective tools, not blanket treatments, and are used only when clinically appropriate.
The Bottom Line
Long COVID cannot be diagnosed—or treated—by shortcuts.
Effective care requires:
- Recognizing Long COVID as a multi-mechanism condition
- Using symptom and trigger patterns to identify causes
- Confirming findings with targeted testing when needed
- Designing individualized, mechanism-based treatment plans
- Adjusting care as the body recovers
This process replaces trial-and-error medicine with strategy—and gives patients a clear, rational path forward.