Epipharyngeal Abrasive Therapy (EAT) For Long COVID
The Japanese Breakthrough: Science-backed protocol from targeted Long COVID recovery.
Quick Answer: Epipharyngeal Abrasive Therapy (EAT) is a 10-15 minute in-office procedure for treating vagus nerve inflammation in Long COVID patients. It reduces inflammatory cytokines (TNF-alpha, IL-6, IL-1) and restores autonomic function by targeting chronic inflammation in the epipharynx (the area behind your nasal cavity where vagus nerve endings reside). Dr. Groysman is one of very few U.S. physicians offering this specialized treatment.
Meet The Vagus Nerve Inflammation Testing Doesn't Catch
You’ve seen multiple specialists. Your bloodwork came back normal. Your throat looks fine (but doesn’t feel fine). Yet here you are, still dealing with persistent symptoms disrupting your daily life.
Epipharyngeal Abrasive Therapy (EAT) targets inflammation in the epipharynx (the area behind your nasal cavity in the back of your throat where vagus nerve endings reside). EAT is one of very few treatments directly addressing vagus nerve inflammation.
EAT has been used in Japan for decades to treat chronic epipharyngitis and related conditions.
Dr. Groysman remains one of very few physicians in the United States offering this treatment.
What is Epipharyngeal Abrasive Therapy?
Epipharyngeal Abrasive Therapy is a minimally invasive procedure addressing chronic inflammation in the epipharynx (the upper portion of your throat located behind the nasal cavity).
The procedure involves:
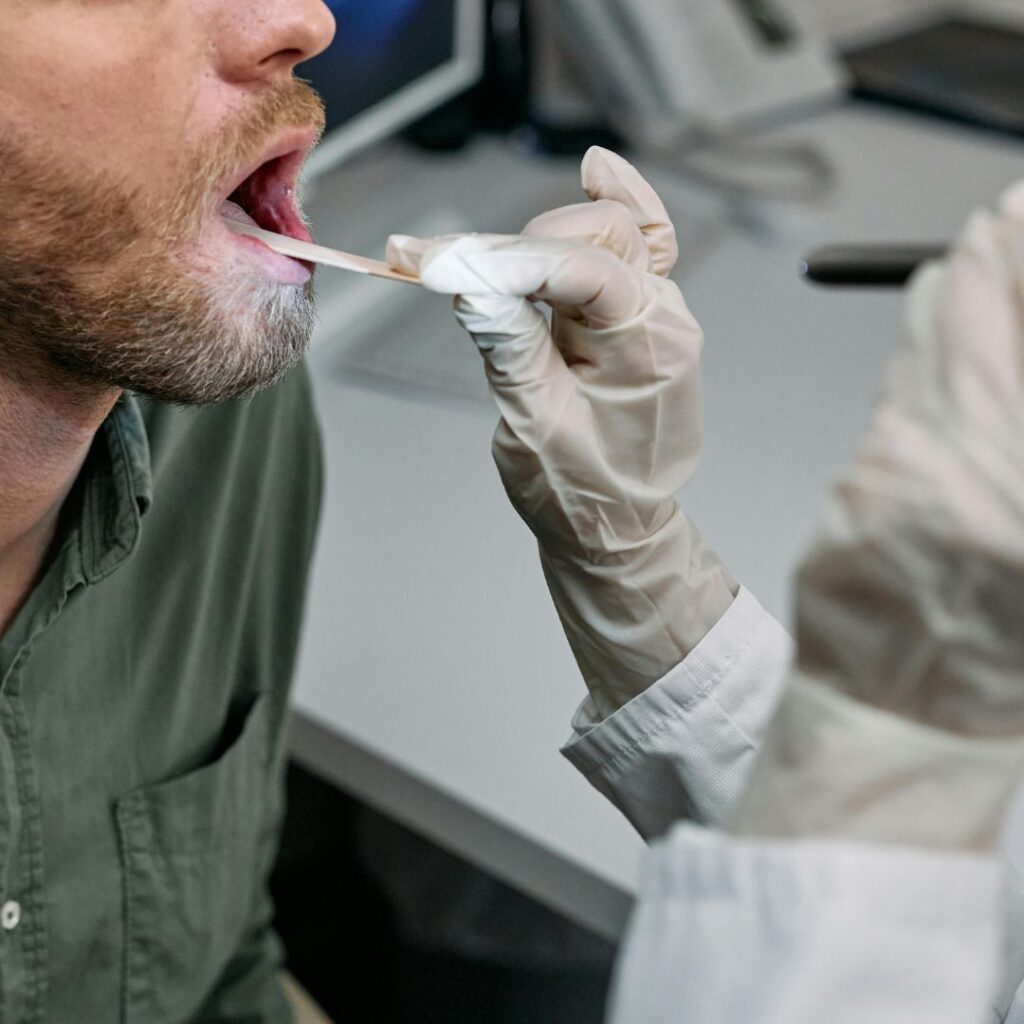
- Gentle mucosal abrasion: A sterile cotton swab soaked in zinc chloride solution is applied to inflamed areas of the epipharyngeal lining under direct endoscopic visualization. This creates controlled minor trauma that stimulates the body’s natural healing response while removing inflammatory debris and biofilms.
- Vagus nerve stimulation: The procedure directly stimulates the vagus nerve playing a key role in regulating autonomic functions and reducing systemic inflammation.
- Cytokine suppression: Clinical research indicates that EAT can lower inflammatory cytokines (such as IL-6 and TNF-alpha) hich are associated with immune dysregulation and chronic fatigue.
The procedure is performed using a flexible endoscope inserted through the nostril. Topical lidocaine spray provides adequate numbing—no injections required. Most patients tolerate the procedure well while awake. The zinc application creates a temporary “whitening effect” on inflamed tissue, indicating reduced inflammation.
How Does Epipharyngeal Abrasive Therapy Treat Vagus Nerve Inflammation?
The Epipharynx-Vagus Connection
The vagus nerve is your body’s primary parasympathetic nerve, it regulates heart rate, digestion, inflammation response, and immune function. When vagus nerve function is impaired by epipharyngeal inflammation, multiple body systems are affected simultaneously.
This explains why Long COVID symptoms often cluster across seemingly unrelated systems: cardiac, neurological, gastrointestinal, and immunological symptoms all trace back to vagal nerve dysfunction.
How Epipharyngeal Inflammation Drives Three Core Mechanisms
1. Dysautonomia (Autonomic Nervous System Dysfunction)
Chronic vagus nerve inflammation impairs parasympathetic tone, creating sympathetic dominance or the constant “fight or flight” state driving tachycardia, blood pressure fluctuations, digestive dysfunction, and anxiety-like symptoms in Long COVID.
2. Neuroinflammation (Brain Inflammation)
Inflamed epipharyngeal tissue releases inflammatory cytokines (TNF-alpha, IL-1, IL-6) which the vagus nerve carries to the brain. This creates the neuroinflammation driving brain fog, headaches, and cognitive dysfunction.
3. Gut Dysbiosis (Microbiome Imbalance)
When vagus nerve function is impaired, gut motility slows, digestive enzyme secretion decreases, and the gut microbiome becomes imbalanced. This explains why many Long COVID patients experience both throat symptoms and gastrointestinal dysfunction. Additionally, 90-95% of serotonin is produced in the gut; this means impaired vagal signaling disrupts serotonin regulation, affecting mood, sleep, and autonomic function.

Who Should Consider Epipharyngeal Abrasive Therapy for Long COVID?
ENT & Respiratory Symptoms:
- On going sore throat and postnasal drip – Direct epipharyngeal inflammation
- Chronic cough, hoarseness, and voice changes – Mucosal inflammation and vagal nerve irritation
- Persistent Nasal congestion – Chronic inflammation affecting nasal passages
- Eustachian tube dysfunction, tinnitus, hearing difficulties – Inflammation affecting middle ear drainage pathways
Neurological Symptoms:
- Pressure headaches unresponsive to usual treatments – Neuroinflammation can affect nerve signals through vagal pathways
- Dizziness, vertigo, and balance issues – Vagal nerve dysfunction can affect vestibular regulation
- Brain fog and difficulty concentrating – Neuroinflammation can occur via vagal inflammatory signaling
Autonomic Symptoms:
- Chronic fatigue and profound exhaustion – Dysautonomia driven by impaired parasympathetic tone
- Mood disturbances and anxiety-like symptoms – Disrupted serotonin regulation through gut-brain axis
- Sleep disturbances: insomnia, snoring, daytime sleepiness – Dysautonomia affecting sleep-wake cycle regulation
Gastrointestinal Symptoms:
- Acid reflux and heartburn – Vagal nerve controls lower esophageal sphincter tone
- Digestive dysfunction and irregular motility – Vagal nerve regulates gut motility and enzyme secretion
If you experience 3 or more symptoms from this list, epipharyngeal inflammation is likely affecting vagus nerve function across multiple systems.
Single isolated symptoms may stem from a combination of six mechanisms, but the cluster pattern indicates vagal involvement and makes EAT a good intervention. The broader your symptom pattern across ENT, neurological, autonomic, and gastrointestinal categories, the more likely epipharyngeal inflammation and vagus nerve dysfunction are central to your Long COVID symptoms.
Is EAT Right for You? Take This Quick Assessment
EAT is most appropriate if:
- Your ENT cleared you with no active infection found
- Standard throat examination showed nothing abnormal
- You have multiple symptoms across ENT, neurological, and autonomic categories
- Symptoms persist despite conventional treatments
- Your testing showed dysautonomia
EAT is NOT appropriate if:
- You have active throat infection or acute COVID (wait 1-2 weeks after recovery)
- You’re seeking immediate symptom relief (this addresses root cause inflammation)
- You have severe bleeding disorders (procedure involves minor mucosal abrasion)
Next Step: Schedule consultation to determine if epipharyngeal inflammation is driving your symptom pattern
What to Expect During Epipharyngeal Abrasive Therapy
Epipharyngeal Abrasive Therapy is performed in-office, typically takes only 10-15 minutes so you’re home the same day. Here’s what you can expect:
- Initial Evaluation: Endoscopic imaging is used to confirm inflammation in the epipharynx. A flexible endoscope (3.8mm diameter) is inserted through your nostril to visualize the epipharyngeal area. This allows Dr. Groysman to identify specific areas of inflammation that require treatment. The endoscope is thin enough to fit through even narrow nostrils.
- Numbing: No injections requited. The inside of your nose and back of your throat are numbed using topical lidocaine spray. The numbing takes effect within a few minutes. Because the procedure is performed through the nose rather than the mouth, you won’t experience gagging during treatment.
- The Treatment: A sterile cotton swab soaked in zinc chloride solution is gently rubbed against the inflamed epipharyngeal tissue. This creates a controlled, gentle abrasion to removes inflammatory debris and stimulate healing. Most patients tolerate the procedure well while awake. If you tend to be anxious, oral sedation can be prescribed to take 30 minutes before the procedure, you’ll remain awake but more relaxed.
- Recovery: Some patients may experience mild soreness or a scratchy throat, which resolves quickly. The intensity depends on how inflamed your epipharynx was initially.
Safety: Backed by decades of Japanese clinical use, EAT has minimal risks and a strong safety profile.


Personalized Care with Dr. Groysman
At Covid Institute, we know every patient’s experience with Long COVID is unique.
This is why Dr. Groysman develops personalized treatment plans tailored to your unique symptoms, which may include:
- Epipharyngeal Abrasive Therapy (EAT) as a primary intervention.
- Supplementation and prescription medications to enhance recovery.
- Complementary therapies to address systemic inflammation, which may include SGB (or Stellate Ganglion Block).
“85% of our patients report marked improvement within the first few sessions. This is based on our own clinical observations conducted in our clinic, not an actual clinical trial.”
Patient Success Stories
Severe Fatigue Recovery
“Dr. Groysman, you are amazing and after getting SGB (both sides) and one EAT, I’ve been continually recovering over the past 5 months. I got LC in March, 2020 and had tremendous fatigue, mostly bed bound, which ruined my life. My immune system was non-existant.” – AEB 12/2024
Singer Recovers Voice
UPDATE: My daughter is a singer and worked with her voice coach yesterday for the first time since her SGB and EAT 2 weeks ago. I got this message from her voice coach today: “I’m so excited to see where these treatments take her. Her voice is already coming back to the way it was. I know it’s hard to tell for you guys probably, but when she started with all of this her range dropped, became super airy in her tone, breath support etc. Yesterday there was already so much more tone!” – J.L. 8/2024
39-Month Journey Ends
“Thank you Dr. Robert for being one big step on my son’s recovery. Today he finally back to his normal happy and energetic, can get up at 7 and go to his hobby Robotics club. It was 39 months journey with more than 50 doctors/therapists. The EAT procedures were able to rid of all the focal inflammation , so he was able to further progress to get rid of the POTS PEM and chronic fatigue. Merry Christmas to you and your team , and all people here ! Do not give up , human body are so magic , we should all be able to heal !” – SS 12/2024
Epipharyngeal Abrasive Therapy FAQ's
Right now, Dr. Groysman is the only physician outside of Japan that offers this procedure on a regular basis.
In general it takes 10-15 minutes to complete the procedure. It takes a few extra minutes to numb up the back of the nose.
We numb the inside of the nose using a topical numbing spray that has lidocaine. The procedure is well tolerated awake by most.
The size of the nostrils doesn’t actually matter. The flexible endoscope camera is 3.8 mm and can fit thru the narrowest of nostrils.
Yes, even kids tolerate this procedure awake. If sedation is required, we can call something oral in before the procedure.
Yes you can have both procedures done on the same day, just not at the same time.
Yes. Its preferable to wait 1-2 weeks after recovering from a cold, flu or COVID before having the EAT procedure.
It may be repeated as many times as needed.
You may experience some discomfort or burning in the back of your nose. The amount depends on how inflamed your epipharynx is. Soreness can last for 1-2 days after the procedure. Using regular saline nasal spray and gargling with salt water (½ teaspoon of salt dissolved in warm water) can reduce discomfort.
It does not. There is no CPT code to bill even for this procedure.
You can. We can call in an oral sedative for you to take 30 minutes before the procedure. You will still be awake but more relaxed for those that tend to be anxious.
Nothing specific is needed. If you have seasonal or respiration allergies, take your usual medications.
It has 4 mechanisms that work:
- direct cleaning from abrasion – kind of spring cleaning of the back of your nose and throat.
- stimulation of the vagus nerve endings
- decreased inflammatory cytokines
- improved dysautonomia symptoms
You may experience some discomfort of burning in the back of your nose. The amount depends on how inflamed your epipharynx is. Soreness typically lasts for 1-2 days after the procedure. One idea to reduce this is to use a regular saline nasal spray and gargling with a 1/2 teaspoon of salt dissolved in warm water.
It will treat any ENT problems such as pressure headaches, face pain, stuffy nose, post nasal drip, as well as those caused by dysautonomia. It may also help with CFS/ME. Dr. Groysman believes that the EAT procedure works synergistically with the SGB procedure. It can treat the missing gaps that SGB misses.
It all depends on how inflamed the epipharynx is initially. Some will d o fine with 1-2. Others will need 4 or more.
In general, Dr. Groysman recommends waiting 5-7 days between procedures to allow the epipharyngeal area to heal between treatments.
It can treat ENT problems such as pressure headaches, facial pain, stuffy nose, and postnasal drip, as well as symptoms caused by dysautonomia. It may also help with CFS/ME. Dr. Groysman believes that the EAT procedure works synergistically with the SGB procedure, treating gaps that SGB may miss.
Related Questions About Long COVID and EAT
Can Long COVID cause chronic sore throat even after the virus clears?
Yes. Chronic epipharyngeal inflammation from COVID infection creates persistent throat symptoms even after the virus clears. Standard throat swabs show no active infection because the issue is inflammatory, not infectious. This is why antibiotics don’t help—there’s no bacteria to kill.
Why does my ENT say nothing is wrong but I still have throat pain?
Standard ENT examination looks for infection or structural damage. When those tests are normal, you’re told you’re fine. But standard ENT doesn’t assess chronic inflammation, vagus nerve function, or inflammatory cytokines driving your symptoms.
What is vagus nerve inflammation and how does it cause Long COVID symptoms?
The vagus nerve is your primary parasympathetic nerve controlling heart rate, digestion, and inflammation. When inflamed, it disrupts autonomic function (dysautonomia), carries inflammatory signals to the brain (neuroinflammation), and impairs gut-brain communication (gut dysbiosis). This explains why Long COVID affects multiple body systems simultaneously.
Where can I get Epipharyngeal Abrasive Therapy in the United States?
As of [year], Dr. Groysman at the COVID Institute is one of very few physicians offering EAT in the United States. The treatment has been used in Japan for decades but remains unavailable at most American Long COVID clinics because standard medical training doesn’t include vagus nerve inflammation assessment.
Schedule a Consultation
If persistent throat symptoms, brain fog, dysautonomia, or chronic fatigue haven’t responded to standard ENT care, schedule a consultation to determine if epipharyngeal inflammation is driving your symptoms and whether EAT is appropriate for your mechanism profile.
References and Additional Reading
EAT is supported by studies showing reduction in inflammatory cytokines and improvement in chronic epipharyngitis symptoms. For comprehensive research references and six mechanism framework, see Dr. Groysman’s book series.